National
Rwanda achieves 2006 Abuja Declaration targets on health
Rwanda is among the six countries that have achieved the recommendations of the 2006 Abuja Declaration of Head of States of African Union countries of allocating to health at least 15 per cent of their annual budget.
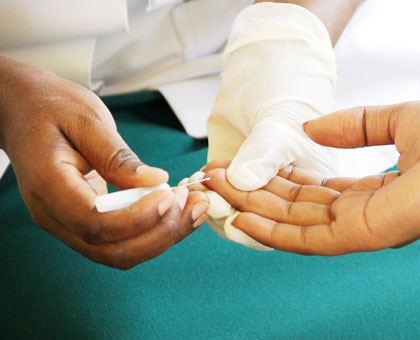
A volunteer testing for HIV at King Faisal Hospital, Rwanda. More than 90 per cent of persons infected with HIV/Aids can now access ARTs that are now available in almost all health fac....
