Health
HIV/AIDS: How to break the bad news
There are two answers to expect when you take an HIV test -- negative or positive. The biggest challenge, however, is how to receive the bad news. That is what healthcare providers are supposed to help patients with.
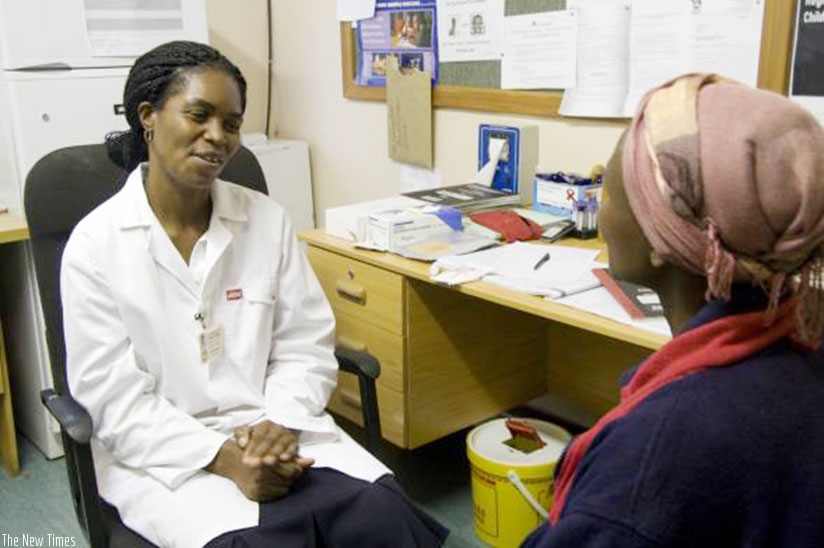
A medic counselling a client before an HIV test is done. / Internet photo.
