Health
Mother and child care week impacts lives at Rutongo Hospital
Silvie Mukundwa, a resident of Masoro sector, Rulindo District, Northern Province, saw her 4-year-old son suddenly develop many symptoms such as running nose, watery eyes, swollen eyelids and sneezing.
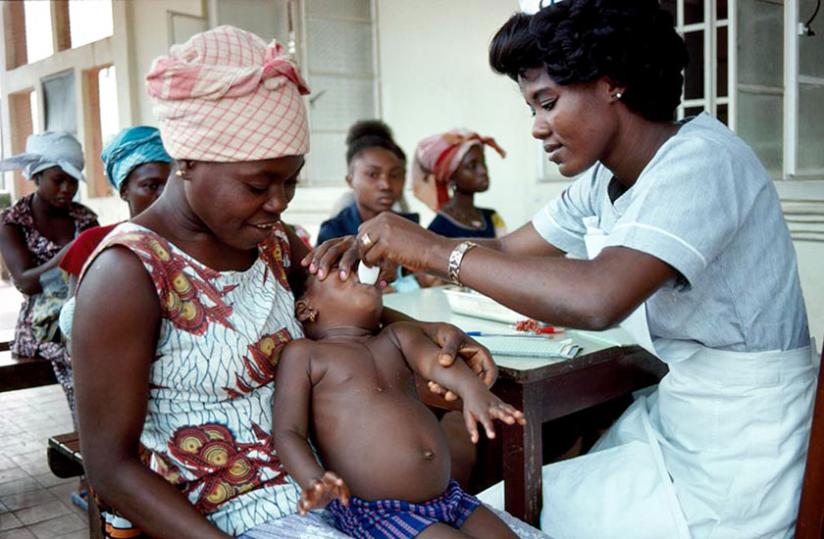
A child is immunised at a health centre. (Net photo)

