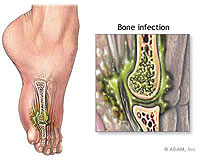
HEALTH : Osteomyelitis – infection of the bone
Germs causing infection and disease can affect any part of the body, including the bones, a condition called osteomyelitis. It becomes different from other kind of infections due to atypical features. It often gets confused with infection of overlying skin and soft tissues. It is also resistant to treatment at times and needs longer duration of treatment.