Insight
Why Ebola is so dangerous
According to the World Health Organisation, evidence suggests the death toll from the Ebola outbreak in West Africa is vastly underestimated. The UN agency said it was prepared for the crisis to continue for months.
The numbers of reported Ebola virus cases and deaths “vastly underestimate the magnitude of the outbreak,” the UN agency said last week.
The death toll from the worst ever outbreak of Ebola has risen to 1,145, WHO said as 76 new deaths were reported in the two days of August 12 and 13 in the four West African nations affected by the epidemic.
The UN health agency said a total of 152 confirmed, probable and suspected new cases of the deadly hemorrhagic fever were reported in the two day period in Guinea, Liberia, Nigeria and Sierra Leone, bringing the total cases for the outbreak to 2,127.
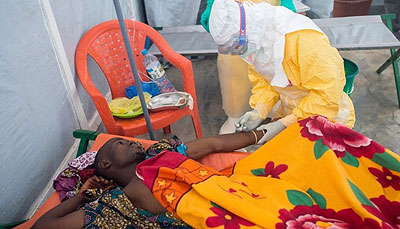
Ebola is a viral illness whose initial symptoms can include a sudden fever, intense weakness, muscle pain and a sore throat, according to the World Health Organisation. Net photo.
