National
Scientists to put lab services at centre of HIV/Aids fight
As the world comes together to try and tackle HIV/Aids, an initiative by the African Society for Laboratory Medicine (ASLM) and UNAIDS is rooting for laboratory services to be placed at the forefront of the fight.
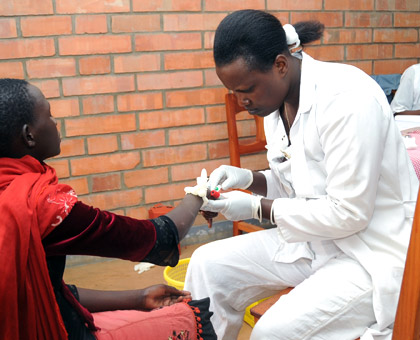
A past voluntary counselling and testing exercise in the country. (File)
