SPONSORED: How early testing, counseling and treatment help in saving lives
The thought of being raped and getting pregnant against your will at an early age can be a horrible experience. It becomes a live nightmare once the woman- the victim- realizes she acquired HIV in the process.
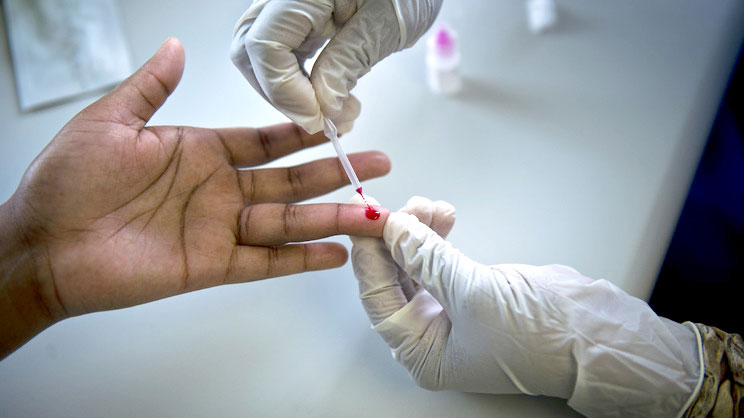
A person being tested for HIV/AIDS.
