WHO Africa boss speaks on status of regional healthcare
Despite the progress made by most countries across the region, the health sector continues to show weaknesses in aspects such as quality, costs and response.
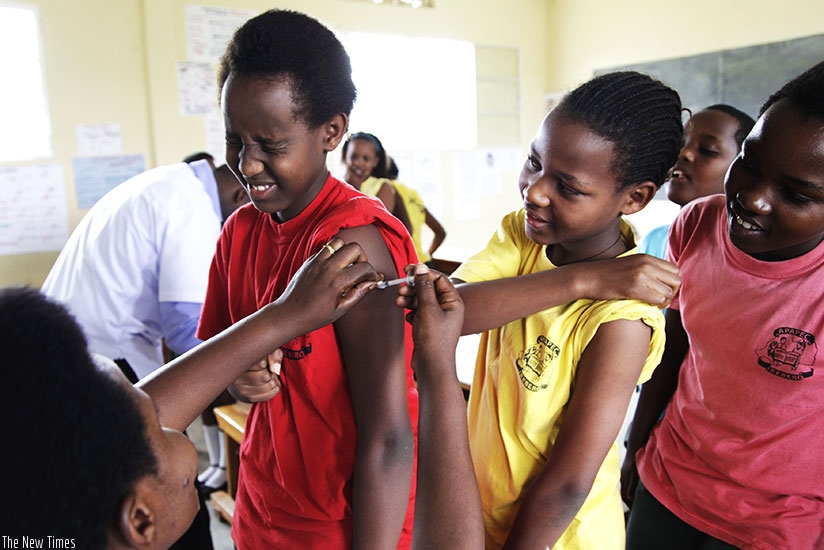
Seraphine Mukanyarwaya, a nurse at Kagugu Health Centre in Kigali, immunises pupils of APAPEC Irebero Primary School. / File

