Health
Successful surgery saves baby born with rare head condition
Alphonsine Mukankuranga carried a normal pregnancy and for nine months she religiously followed the antenatal schedule given by her attendants at Rukara Health Centre, Kayonza District in Eastern Province.
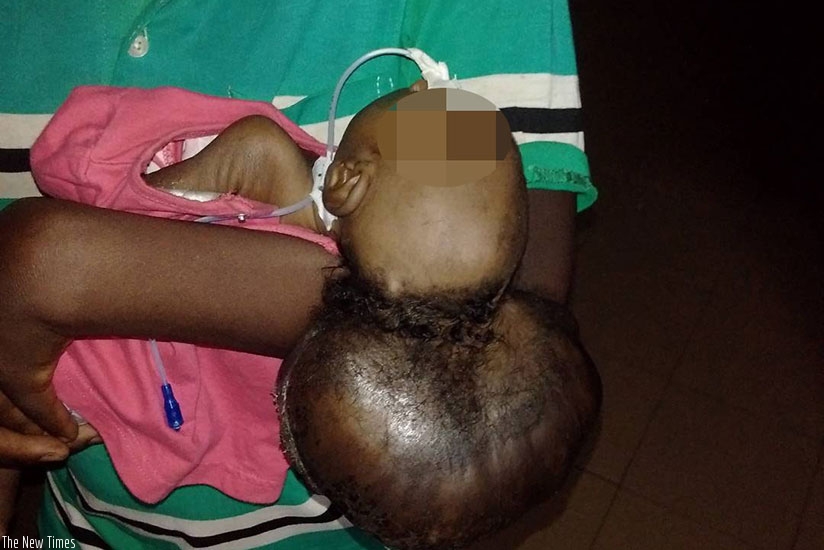
Mukankuranga and baby Ester Niyigena at CHUK before the operation. / Photo by Kelly Rwamapera.
