WHO issues new Hepatitis B guidelines
The World Health Organisation has issued guidelines to simplify diagnosis and treatment of Hepatitis B. The new guidelines come one year after the United Nation’s health agency published the first ever rules on treating Hepatitis C.
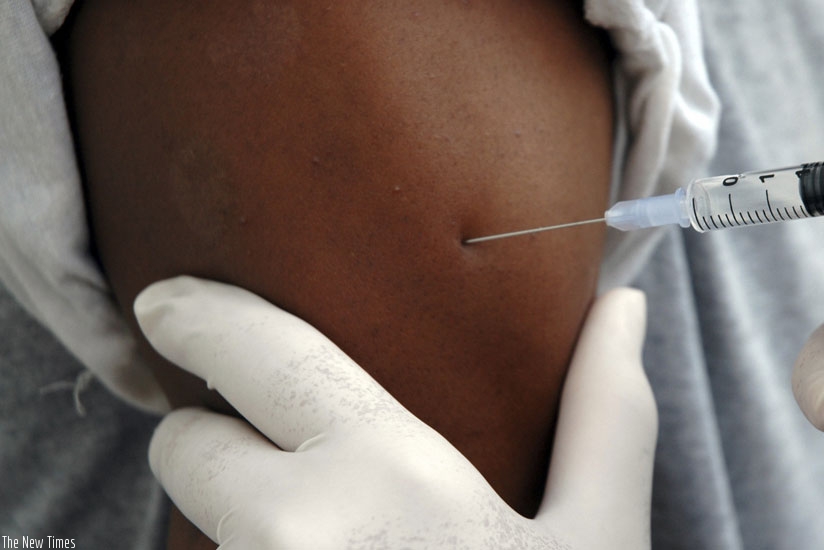
A woman gets a vaccine against Hepatitis B.

