Health
What you should know about celiac disease
If you usually take wheat products, and other kinds of food that contain gluten, it is high time you changed your diet because you could be risking catching celiac disease.
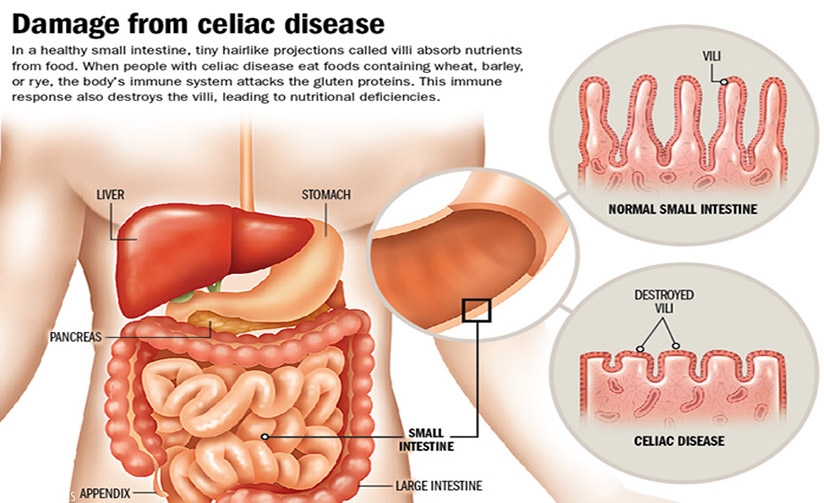
A graphic illustration of how celiac disease affects the intestinal lining. / Net photo.
